Gastric and duodenal peptic ulcers are the cyclical appearance of peptic ulcers in the stomach or duodenum. Peptic ulcer is a defect of the mucosa accompanied by inflammatory infiltration and necrosis. In most cases, the location of the ulcer is the duodenal bulb and stomach, although they can also occur in the lower esophagus and duodenal loop.
Causes of peptic ulcer disease
The most common causes of peptic ulcer disease include Helicobacter pylori infection and nonsteroidal anti-inflammatory drugs (NSAIDs).
Helicobacter pylori is responsible for 75–90% of duodenal ulcers and about 70% of stomach ulcers. Infection occurs through the oral route. Initially, the bacterium causes an inflammatory response and increases the secretion of gastrin, a hormone which leads to a greater production of hydrochloric acid. The acute phase of inflammation can go into the chronic phase, resulting in atrophy of the mucosa and acidity.
In the adult population, the incidence of Helicobacter pylori is high, around 80%, but not all infected have gastric or duodenal ulcers.
The second most common cause of stomach and duodenal ulcers are medications, mainly non-steroidal anti-inflammatory drugs (NSAIDs). These are commonly used painkillers, antipyretics and anti-inflammatory agents, e.g. aspirin, diclofenac, ibuprofen, ketoprofen.
Genetic factors, smoking and blood group 0 are also less likely to develop gastric and duodenal ulcers.
What are the symptoms of peptic ulcer disease?
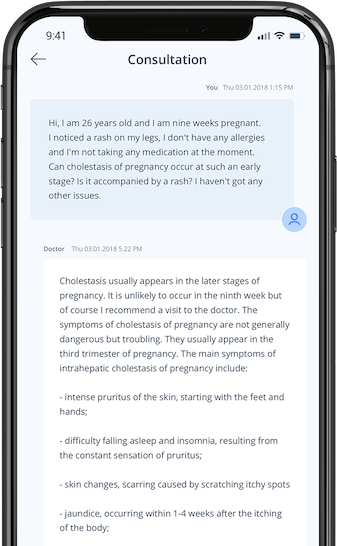
The main symptom of gastric and/or duodenal ulcers is epigastric pain or discomfort, usually on an empty stomach (often at night or in the morning) or 1-3 hours after meals and disappears after ingesting food or taking antacids. The disease can also be manifested by a feeling of "fullness" or spread after meals, nausea, belching, heartburn, or vomiting. The course can also be quite asymptomatic.
How do you recognize it?
The most important examination performed in the course of gastric and duodenal ulcer diagnostics is endoscopic examination - gastroscopy. It allows confirming the disease, detecting the presence of Helicobacter pylori and taking specimens for diagnostic tests: rapid urease test (a tissue section taken during gastroscopy is placed on a special disc containing urea and a dye that changes color in the presence of urease - an enzyme produced by H. pylori - a change in color confirms the presence of urease, and thus the bacteria producing this enzyme), histopathological examination (examination under a microscope) or bacterial culture.
Non-invasive tests for detection of Helicobacter pylori include:
- 13C carbon breath test,
- test for detection of Helicobacter pylori antigens in stool,
- a blood test for antibodies to Helicobacter pylori.
It should be remembered that the above tests detect bacterial infection, not gastric and duodenal ulcers.
When should I contact a doctor?
If you have chronic abdominal pain, recurrent nausea, vomiting, or a nagging feeling of fullness, you should see a primary care physician for basic diagnostics for gastric and duodenal ulcers.
How do we treat peptic ulcers?
General recommendations include regular meals, excluding meals that exacerbate or cause discomfort, smoking cessation, and the avoidance of certain medications (acetylsalicylic acid and other NSAIDs).
The main treatment method for peptic ulcers in those infected with helicobacter pylori bacteria is its removal (eradication) by the use of antibiotic therapy and gastric acid-secreting drugs. A doctor will decide the appropriate treatment regime.
Relief may be provided by over-the-counter antacids or histamine H2 blockers (famotidine, ranitidine).
Proton pump inhibitors (esomeprazole, lansoprazole, omeprazole, pantoprazole), which inhibit the production of hydrochloric acid, are more effective. However, these medicines should be taken as prescribed.
Surgical treatment usually involves treating complications of gastric and duodenal ulcers.
Complications of peptic ulcer disease
In the course of gastric and duodenal ulcer disease, serious complications can occur. Bleeding hemorrhage can potentially be life-threatening, while chronic bleeding can lead to anemia due to iron deficiency. Scars forming in the area of healed ulcers, mainly gastro-duodenal junction, can lead to mechanical obstruction, preventing the gastrointestinal tract from moving to the distal sections of the gastrointestinal tract. Another dangerous complication is the perforation (i.e. perforation) of the stomach or duodenal wall by an ulcer, which is an indication of urgent surgical intervention.
ATTENTION!
In the event of:
- vomiting with any visible blood or a "coffee-like" appearance
- black, tarry stools
- signs of shock (weakness, drop in blood pressure, cold, sweaty skin)
- severe stomach pain accompanied by abdominal muscle tension
you should immediately report to a doctor or to the Hospital Emergency Department, because hospitalization is necessary in such cases.
- Internal Szczeklik 2018 Internal Medicine Handbook, Authors: Piotr Gajewski, Andrzej Szczeklik Publisher: Medycyna Praktyczna
- https://www.mp.pl/pacjent/gastrologia/choroby/zoladek/63409,choroba-wrzodowa-zoladka-i-dwunastnicy
- https://www.mp.pl/pacjent/gastrologia/lista/95973,zalecenia-dotyczace-leczenia-zakazenia-helicobacter-pylori