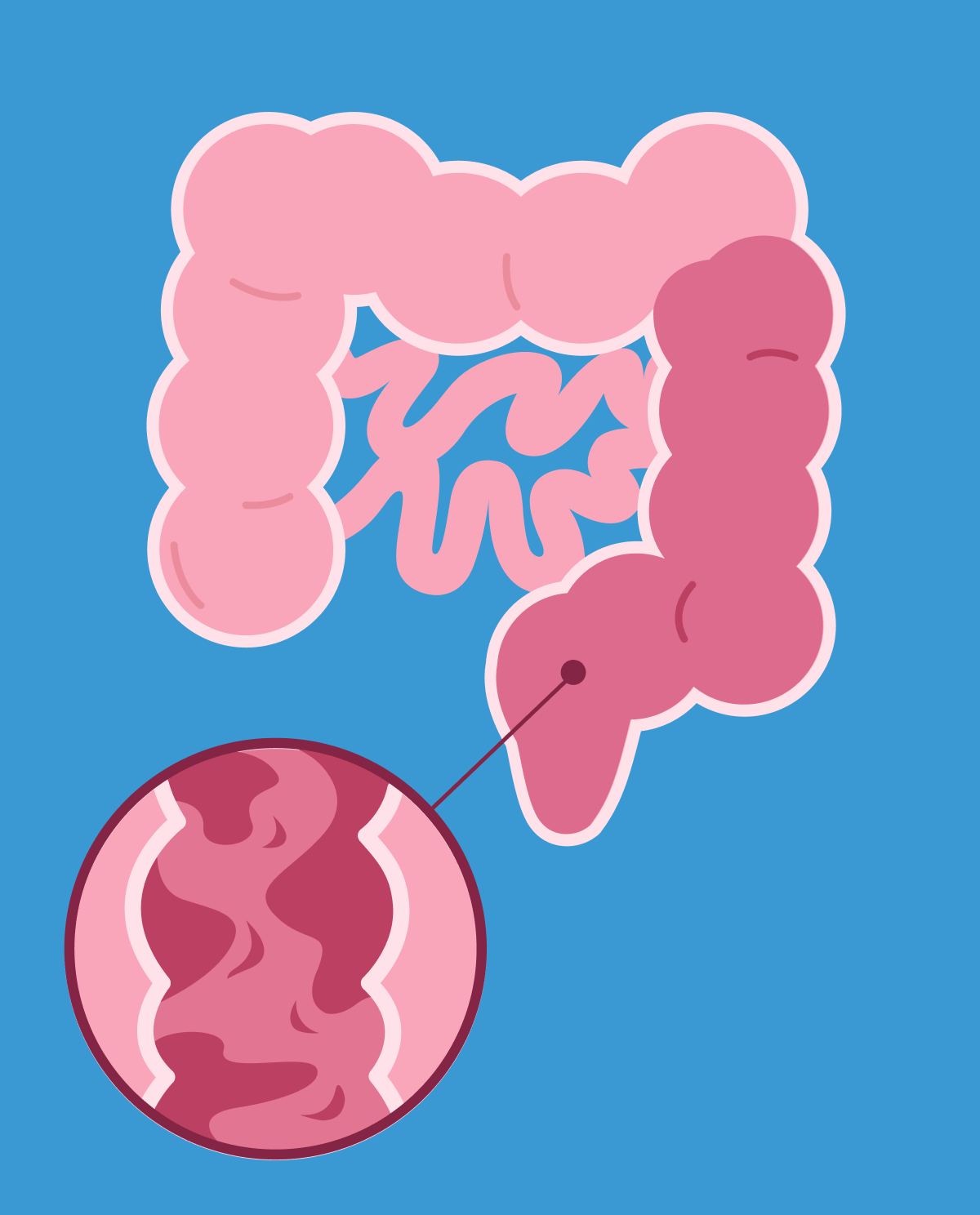
Research has shown that at any point in time depending on the definition used (self-diagnosis or functional diagnosis), constipation affects between 1 in 6 to 1 in 10 people globally. Constipation most commonly occurs when stool movements are too slow within the colon and thus cannot be eliminated via the rectum resulting in hardening of the stools.
Constipation is medically defined as infrequent (less than three) passages a week or painful passing of stools that persists for several weeks. In this short article, I will outline the different types of constipation, symptoms associated with constipation, treatment modalities used, and prevention.
Types of constipation
Primary constipation
Also known as idiopathic or functional, this type of constipation is the primary problem and isn’t secondary to another illness.
- Normal transit constipation: the most common form of constipation seen by physicians. Studies have shown a normal rate of stool passage but the patient ‘feels’ constipated. In addition to this feeling, various symptoms have been reported such as hard stools, bloating, and abdominal discomfort/pain. Various studies have associated this type of constipation with IBS (inflammatory bowel syndrome).
- Slow transit constipation: This type of constipation is a result of diminished / impaired peristalsis (motor propulsion of food and waste by the gastrointestinal tract) resulting in the slow passage of stool. The following has been more prevalent in women.
- Outlet constipation: results from pelvic floor muscle dysfunction. The pelvic floor muscles support the adequate function of the uterus, bladder, and bowel. Damage can occur as a result of childbirth or any traumatic event to the nerves supplying the pelvic floor. Patients report delayed bowel emptying due to pain, and hand assistance to induce bowel movement.
Secondary constipation
Constipation arises as a result of surgery, medication, or primary illness. The most common cause of secondary constipation include the following:
- diabetes,
- depression, eating disorder,
- certain medications (opioids, antidepressants, anticholinergic medication, NSAIDs, anesthesia, and so on),
- hypothyroidism,
- irritable bowel syndrome.
Less common causes of secondary constipation include the following:
- nervous system disruptive illnesses such as multiple sclerosis,
- spinal cord injuries,
- stroke,
- anal fissure,
- colon cancer,
- vitamin and mineral deficiency ( vitamin C, B12, Magnesium).
Symptoms
- having hard lumpy stools,
- fewer than three stool passages a week,
- painful defecation,
- feeling of blockade and pressure in the rectum,
- incomplete emptying,
- need to use your hand to press on your lower abdomen to exert pressure or use a finger to remove feces.
Risk factors associated with constipation
- being a woman,
- poor hydration,
- diet low in fiber,
- being older,
- little to no physical activity,
- medications,
- hormonal imbalance,
- mental health disorders,
- laxative dependence.
Diagnosis
Doctors usually base their diagnosis on complete patient history and physical examination. When the cause remains unknown, a physician can request the following but are not limited to:
- Blood tests: low thyroid function, high calcium levels.
- Sigmoidoscopy: (a flexible tube inserted in the rectum to visualize the lower part of the colon) or a colonoscopy to visualize the entire colon. This type of diagnostic test is very important if the constipation is sudden or if the patient tested positive for occult blood in stools.
- Abdominal X-ray: that can detect bowel obstruction.
- Rectal muscle coordination: can be measured via a procedure called anorectal manometry. In this procedure, a flexible tube is inserted into the anus and rectum. A small balloon is inflated at the tip of the tube and the tube is pulled back through the anal sphincter.
- Colonic transit study: a small capsule containing a wireless recording device or a radiopaque marker is swallowed by the patient and its movements are recorded over 24 to 48hours.
Treatment:
-
Diet and lifestyle changes
- increase fiber intake by eating more fresh fruits and vegetables,
- exercise regularly,
- when you feel the urge to defecate, don’t ignore it.
-
Laxatives
- tap enemas (over the counter) and suppositories (example: Bisacodyl or glycerin) which aid in lubrication,
- stool softeners (docusate calcium or docusate sodium) work by drawing in more water to soften the stool,
- fiber supplementation (psyllium, methylcellulose) used to bulk stool,
- stimulants such as sennosides or bisacodyl stimulate intestinal peristalsis,
- osmotic laxatives include lactulose, polyethylene glycol, oral magnesium hydroxide, and so on - the following draw more water from the body to soften stool and facilitate bowel movement.
- https://www.thelancet.com/journals/langas/article/PIIS2468-1253(21)00111-4/fulltext
- https://www.mayoclinic.org/diseases-conditions/constipation/symptoms-causes/syc-20354253
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3170709/
- https://onlinelibrary.wiley.com/doi/full/10.1111/j.1440-1746.2006.04333.x