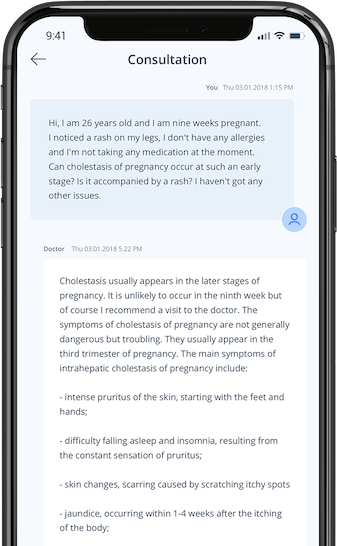
Open communication about medical issues is vital for effective doctor-patient relationships. Doctors rely on patients to share their symptoms, health behaviors, and emotional well-being. This information helps clinicians diagnose and recommend appropriate treatments. If patients withhold or misrepresent details, the advice and decisions made by doctors may not be in the patient's best interest. While it's essential for patients to provide accurate information, there's a prevailing belief in the medical field that patients sometimes withhold the truth. Limited research suggests that a significant number of patients might not share essential details with their doctors. For instance, data from the Health Information National Trends Survey (HINTS) revealed that over 12% of patients have, at some point, withheld information from a clinician due to concerns about the confidentiality of their medical data.
Common "Taboo" Topics
- Urinary Incontinence: This refers to the unintentional leakage of urine. While common among the elderly, it can affect adults of all ages. The actual prevalence might be higher than reported, as some patients may not discuss it with their doctors. The condition's prevalence ranges from 5% to 70%.
- Erectile Dysfunction (ED): Previously termed impotence, ED is the inability to maintain a firm erection for sexual activity. It can be a sign of various underlying issues. The global prevalence of ED ranges from 3% to 77%.
- Hemorrhoids: These are swollen cushions in the rectal area. They can result from factors like prolonged constipation. Hemorrhoids can cause blood vessels to enlarge, altering the tissue structure in the affected region.
- Bad Breath (Halitosis): Halitosis refers to unpleasant breath odor. It can affect social interactions and self-esteem. The global prevalence of halitosis ranges from 22% to 50%.
- Sexual History/Activity: Providing an accurate sexual history helps doctors assess risks for sexually transmitted infections and promote safe sexual practices. However, discussing sexual history can be challenging due to cultural norms and personal discomfort.
- Gastrointestinal Issues: Conditions like diarrhea and chronic flatulence can be sensitive topics. They can result from various causes, including lactose intolerance and irritable bowel syndrome.
- Mental Health: Depression is the most common severe mental health issue among primary care seekers. Research shows that those with more severe symptoms are more likely to be diagnosed.
Why Patients Might Hesitate
Several reasons might deter patients from discussing "embarrassing" symptoms with their doctors:
- Cultural Norms: Cultural values can dictate what topics are appropriate for discussion.
- Fear: Patients might worry that discussing certain issues will lead to judgment, affecting their self-esteem.
- Communication Barriers: Patients might struggle to describe their symptoms, fearing misinterpretation or dismissal.
- Past Negative Experiences: Previous unfavorable interactions with healthcare professionals might deter open communication.
- Taboos: Some topics, especially those related to sexual or gastrointestinal issues, might be considered taboo in certain cultures.
- Lack of Awareness: Some patients might not realize the importance of sharing certain information.
Encouraging Open Communication
To foster open communication, healthcare providers should:
- Build Trust: Trust is foundational for open patient-provider communication.
- Use Clear Language: Avoiding complex medical jargon and explaining concepts in layman's terms can make patients feel more at ease.
- Listen Actively: Providers should listen attentively, ask clarifying questions, and show empathy, assuring patients that their concerns are valid and will be addressed.
- Association of Statin Use With All-Cause and Cardiovascular Mortality in US Veterans 75 Years and Older
- The feasibility of using electronic health records (EHRs) and health information exchange systems for population health surveillance
- Urinary Incontinence in Older Adults
- Erectile Dysfunction Overview
- The Association Between Physical Activity and Risk of Mortality Is Modulated by Grip Strength and Cardiovascular Health: Biomarker Data from UK Biobank
- Erectile Dysfunction
- Halitosis: Current concepts on etiology, diagnosis and management
- Halitosis: Current concepts on etiology, diagnosis and management
- Halitosis
- Halitosis: An overview of epidemiology, etiology and clinical management
- Epidemiology of erectile dysfunction: a systematic review and meta-analysis
- Halitosis: A review of associated factors and therapeutic approach
- Who Is at Risk of Nondetection of Mental Health Problems in Primary Care?