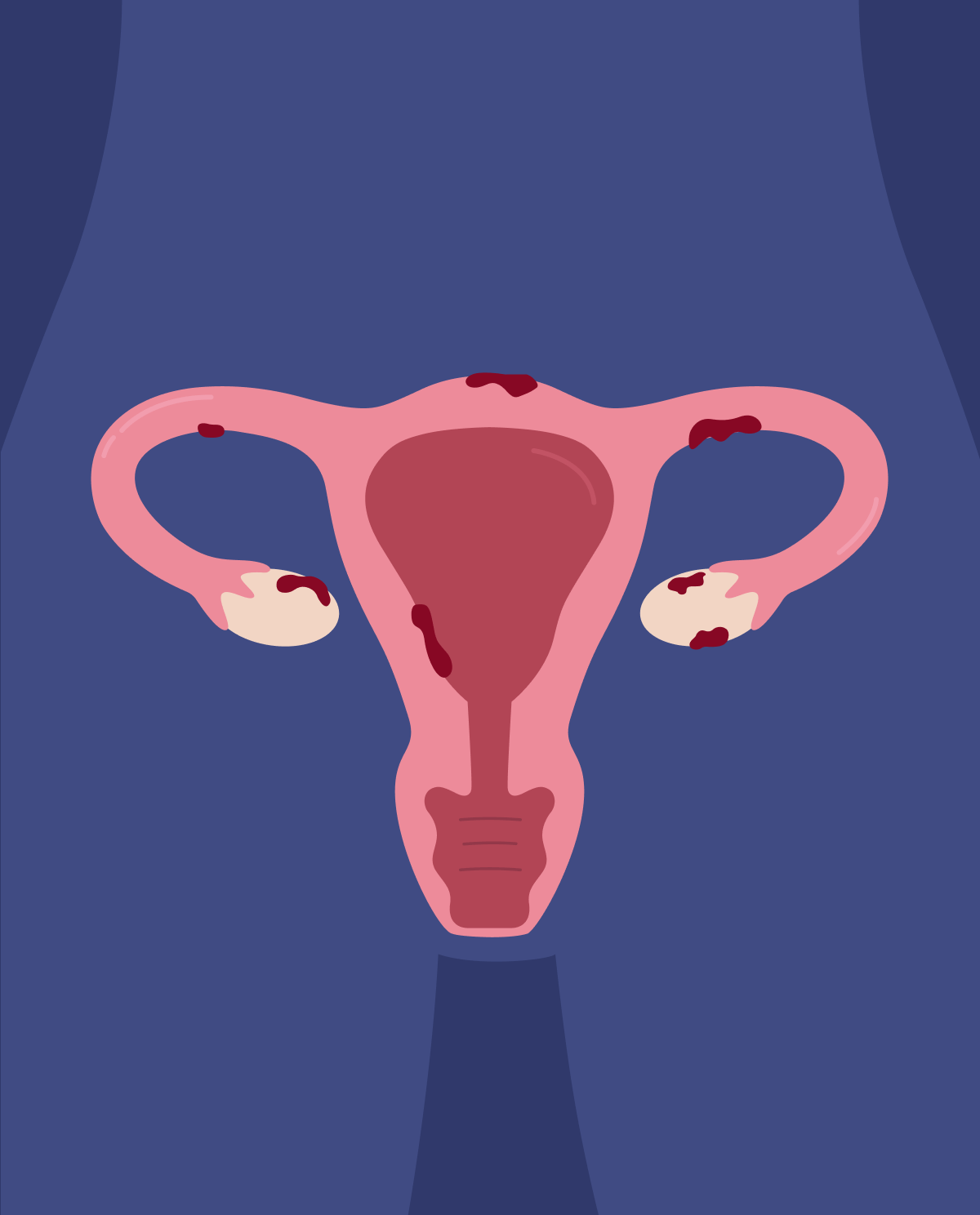
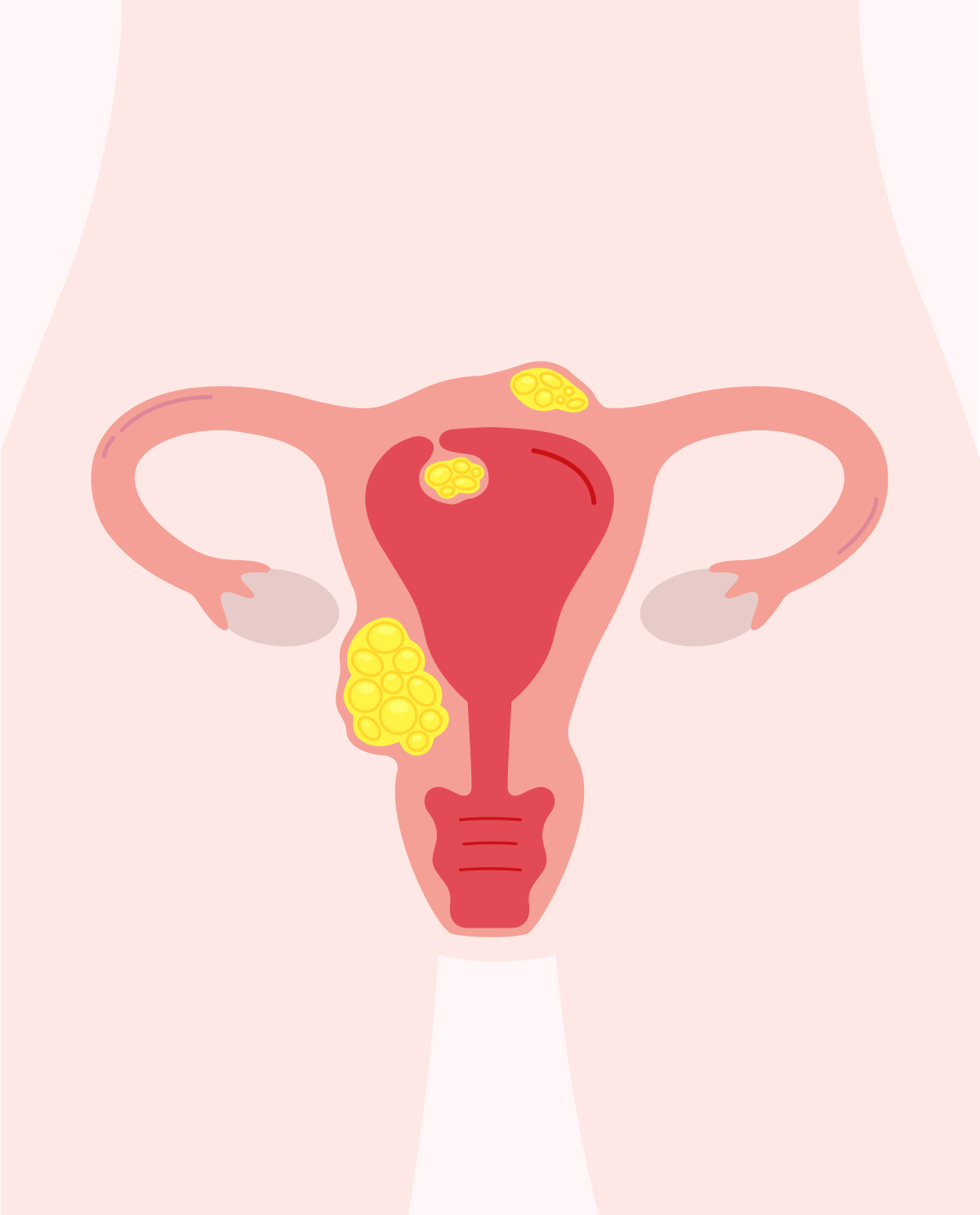
Pelvic inflammatory disease or PID is an inflammatory process of the reproductive organs in women. PID most commonly results from bacterial infections acquired during intercourse, mainly chlamydia, and gonorrhea. At other times, it can result from bacteria entering the uterus during instances when the cervical barrier is disturbed (i.e., after abortion, miscarriage, or childbirth). The disease results from what we call an "ascending" infection thus spreading from the lower genitalia (i.e., vagina) to the upper genitalia (i.e., Uterus, fallopian tubes, and ovaries).
Risk factors
- history of PID and/or STI (sexually transmissible infections),
- being sexually active/ unprotected,
- unprotected sex with multiple sexual partners,
- regular douches can induce an imbalance in bacteria thus facilitating ascending infections.
Symptoms associated with PID
As with other diseases, symptoms severity varies from person to person. Symptoms could range from inapparent to mild to severe. When women experience symptoms, the following are the most widely reported:
- fever and chills,
- difficult urination (urinary hesitancy) and/or painful urination (dysuria),
- painful intercourse,
- heavy vaginal discharge with a foul odor,
- bleeding between periods and/or during or after intercourse,
- pain localized in the pelvis and abdomen,
- nausea / vomiting.
Complications of PID
If left untreated, the inflammatory processes during PID can induce the formation of scar tissue and abscesses in the reproductive tract which can result in the following:
- infertility,
- chronic pelvic pain that can last months to years,
- ectopic pregnancy.
Diagnostic methods
There is no single test that provides a concrete diagnosis of PID, your primary healthcare provider will first focus on the history taking and the physical examination. PID would be suspected by your primary healthcare provider when you present with lower abdominal pain/ pelvic pain with or without the symptoms mentioned above.
- Pelvic examination: the pelvis will be examined by the physician for tenderness (pain) and/or swelling. During this examination, samples of vaginal discharge will be tested for the most common bacterial pathogens,
- Ultrasonography,
- Blood / urine tests,
If the diagnosis remains unclear, your primary healthcare provider might request an endometrial biopsy (to test for infectious agents) or laparoscopic examination to visualize your internal organs.
Treatment for PID
Early diagnosis and treatment are key to preventing the development of complications. If scarring has already occurred, it is not possible to reverse the damage induced by inflammation.
- antibiotics,
- if your blood work/vaginal discharge was positive for bacterial infection, your partner should get antibiotics as well,
- abstinence until treatment completion,
- If you haven’t responded to oral therapy or are pregnant, you may need to be hospitalized to receive intravenous antibiotics. In rare occurrences, if an abscess isn’t responding to treatment while in the hospital, you may require surgical removal as rupture of the abscess could cause a life-threatening situation.
Tips on prevention
- avoid douches,
- both partners should be tested,
- practice safer sex,
- speak to your primary healthcare provider about contraception.